Nerve Conduction Work-Ups
...
In routine clinical work, certain sets of nerve-conductions must be studied in evaluating peripheral nervous system function. These sets depend on the nature of the patient’s problem and their referral diagnosis.
General guidelines can usually be prepared for performing a given work-up for a specific group of diseases. These guidelines need to meet two requirements:
– General enough to include most of the abnormalities seen in this group
– Flexible enough to allow adjustments as needed.
Five general work-ups are described: routine upper extremity, routine lower extremity, generalized neuropathic process, myopathy, and neuromuscular junction.
Routine Upper Extremity
This work-up is for the study of root or plexus lesions and compression/entrapment or traumatic neuropathies of the upper extremity.
The work-up consists of:
– Median sensory and motor studies with F-waves
– Ulnar sensory and motor studies with F-waves
– Radial sensory study
Routine Lower Extremity
This work-up is for the study of root or plexus lesion and compression/entrapment or traumatic neuropathies of the lower extremity.
The work-up consists of:
– A sural sensory study
– A superficial peroneal sensory study
– A peroneal motor study with F-waves
– A posterior tibial motor study with F-waves
– H- refelx studies in peripheral neuropathies and suspected lumbosacral root lesions
Generalized Neuropathic Process
This work-up is for the study of generalized sensory/motor peripheral neuropathies and disease processes involving the anterior horn cell.
The work-up consists of:
– A routine upper extremity (see above)
– A routine lower extremity (see above)
– H-reflex studies
Myopathy
This work-up is for the study of the muscle diseases and myotonias.
The work-up consists of:
– A limited routine upper extremity work-up (median sensory and motor studies)
– A limited routine lower extremity work-up (sural sensory and peroneal motor studies)
Only limited studies are performed because the proximal nature of the disease results in a low yield on nerve conduction studies.
NeuromascularJunction
This work-up is divided into presynaptic (for diseases such as Lambert-Eaton, botulism) and postsynaptic (for diseases such as myasthenia gravis).
Presynaptic neuromuscular junction work-up: Limited routine upper and lower extremity work-ups are done. In Lambert-Eaton syndrome, low motor amplitudes are present diffusely. A muscle with a particularly low amplitude is chosen and a postexercise (post-tetanization) study is performed: ask the subject to exercise the affected muscle against resistance for ten seconds. Then stimulate the nerve once. Typically the pre-exercise response has an extremely low amplitude, in the order of .5 to l mv. Immediately after exercise the amplitude is significantly increased, at least by 100 percent over the pre-exercise level, and commonly by 200 to 300 percent. The facilitation thereafter decreases slowly and the response regains its pre-exercise level in about three minutes. Slow (2-3 Hz) repetitive stimulation causes a small decrement of the response.
Postsynaptic neuromuscular junction work-up: Limited routine upper and lower extremity work-ups are done and slow repetitive stimulation (2 pulses per second x 4 or 9 depending on equipment used) are done on a distal foot or hand muscle at first, and, if negative, on a proximal upper extremity muscle. Take extra care to ensure that the temperature of the limb under study is no less than 35 degrees; cooler temperatures may artificially repair a decrement on repetitive stimulation.
Slow 2-3 Hz repetitive stimulation is performed before and after exercise during a three-minute period. Adequate immobilization of the limb under study is essential as minimal displacement of the baseline may give a false decrement.
To begin, stimulate the nerve under study four times in a row at a frequency of 2 pulses per second. The baseline of all four potentials must be strictly superimposed. A decrease in the amplitude or area of more than 10 percent between the first and fourth potential is interpreted as a positive decrement (Figure 63).
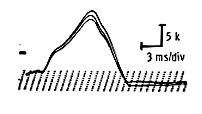
Next, ask the subject to exert the muscle under study against resistance for 30 seconds. Immediately thereafter, stimulate the nerve repetitively four times. Perform these repetitive stimulations at 30-second intervals for three minutes. Typically a myasthenic response will show a pre-exercise decrement between the first and fourth response exceeding 10 percent. This decrement is partially and at times totally corrected immediately after exercise. Gradually, however, it reappears and becomes maximal after two minutes, at which point it exceeds the pre-exercise level.
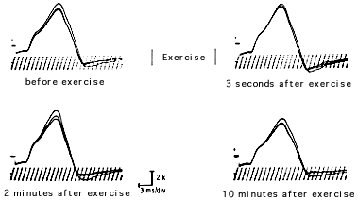
When a distal muscle shows no decrement with the pre- and postexercise repetitive stimulations, a proximal muscle study is mandatory. The study can be performed on the deltoid, biceps, or trapezius. Proximal nerve stimulation requires the use of higher stimulation strengths and longer stimulus duration. They cause a good deal of discomfort and most produce excessive limb displacement. Adequate baseline superimposition is difficult under these circumstances. In about 20 or 30 percent of myasthenics with general symptoms, both distal and proximal slow repetitive stimulation studies may be normal.
