The H-Reflex And F-Wave
...
H-Reflex
The H-reflex is the electrical equivalent of the monosynaptic stretch reflex and is normally obtained in only a few muscles. It is elicited by selectively stimulating the Ia fibers of the posterior tibial or median nerve. Such stimulation can be accomplished by using slow (less than 1 pulse/second), long-duration (0.5-1 ms) stimuli with gradually increasing stimulation strength.
The stimulus travels along the Ia fibers, through the dorsal root ganglion, and is transmitted across the central synapse to the anterior horn cell which fires it down along the alpha motor axon to the muscle. The result is a motor response, usually between 0.5 and 5 mv in amplitude, occurring at low stimulation strength, either before any direct motor response (M) is seen or with a small M preceding it. Understandably, the latency of this reflex is much longer than that of the M response, and a sweep of 5-10 ms/division is necessary to see it.
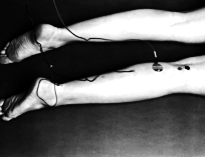
The H-reflex can normally be seen in many muscles but is easily obtained in the soleus muscle (with posterior tibial nerve stimulation at the popliteal fossa), the flexor carpi radialis muscle (with median nerve stimulation at the elbow), and the quadriceps (with femoral nerve stimulation).
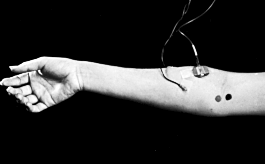
Typically, it is first seen at low stimulation strength without any motor response preceding it. As the stimulation strength is increased, the direct motor response appears. With further increases in stimulation strengths, the M response becomes larger and the H-reflex decreases in amplitude. When the motor response becomes maximal, the H-reflex disappears and is replaced by a small late motor response, the F-wave.
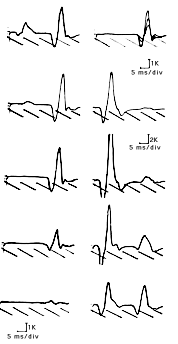
H-reflex latency can be determined easily from charts, according to height and sex or from published normal values. Whatever these values however, the best normal value in localized processes is the patient’s asymptomatic limb. If no facilitation maneuvers are performed, the difference in latency between both sides should not exceed l ms.
The H-reflex is useful in the diagnosis of S1 and C7 root lesions as well as the study of proximal nerve segments in either peripheral or proximal neuropathies.
Its absence or abnormal latency on one side strongly indicates disease if a local process is suspected. Much controversy remains, however, on whether its absence bilaterally in otherwise asymptomatic individuals is of any clinical significance.
F-Wave
The F-wave is a long latency muscle action potential seen after supramaximal stimulation to a nerve. Although elicitable in a variety of muscles, it is best obtained in the small foot and hand muscles. It is generally accepted that the F-wave is elicited when the stimulus travels antidromically along the motor fibers and reaches the anterior horn cell at a critical time to depolarize it. The response is then fired down along the axon and causes a minimal contraction of the muscle. Unlike the H-reflex, the F-wave is always preceded by a motor response and its amplitude is rather small, usually in the range of 0.2-0.5 mv.

The F-wave is a variable response and is obtained infrequently after nerve stimulation. Commonly, several supramaximal stimuli are needed before an F-response is seen since only few stimuli reach the anterior horn cell at the appropriate time to depolarize it. With supramaximal stimulation however, depolarization of the entire nerve helps spread the stimulus to the pool of anterior horn cells thus enhancing its chances to reach a greater number of anterior horn cells at the critical time and produce an F-wave.
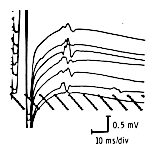
Because different anterior horn cells are activated at different times, the shape and latency of F-waves are different from one another. Conventionally, ten to twenty F-waves are obtained and the shortest latency F-wave among them is used.
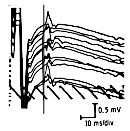
The normal values can be determined from charts or published data and, in unilateral lesions, the best normal values remain those of the patient’s asymptomatic limb. The difference between both sides’ shortest latencies should not exceed l ms.
The data obtained from the F-wave have been used in many different ways to determine proximal or distal pathology. Those include the F-wave chronodispersion or difference in latency between the F-wave with the shortest and that with the longest latency, and the F-wave ratio. We find the F-wave ratio very useful in routine clinical work. It is obtained by dividing the conduction time of the proximal nerve segment by that of the distal nerve segment and is performed as follows:
Obtain the F-wave latency from proximal (F prox) stimulation (knee or elbow). Obtain the motor response likewise from proximal stimulation (M prox). Then determine the latency of the proximal nerve segment by this equation:
Proximal latency = (Fprox – Mprox – 1 ms) / 2
where l ms is the estimated delay encountered by the stimulus at the anterior horn cell.
The latency of the distal segment is none other than the motor response latency obtained from proximal stimulation (M prox).
The F-ratio is then obtained by dividing the proximal latency by the distal latency:
F-ratio = (Fprox – Mprox – 1 ms) / 2 x Mprox
Normal F-wave ratios are obtained from published data (Table XVIII).
The F-wave ratio can be used as follows:
With normal routine conduction velocity:
– A normal F-ratio indicates normal distal and proximal segments
– A decreased F-ratio indicates a distal nerve lesion or entrapment (such as carpal tunnel)
– An increased F-ratio indicates proximal slowing
With slowed routine conduction velocity:
– A normal F-ratio indicates equal proximal and distal slowing
– A decreased F-ratio indicates a normal proximal segment
– An increased F-ratio indicates a predominant involvement of the proximal nerve segment
